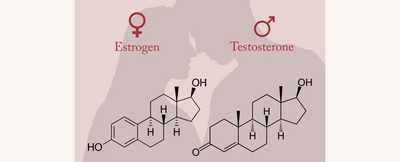
Hormones and Sexual Desire
Your hormones and your sex drive are intricately linked—and it’s well known that the hormonal fluctuations caused by pregnancy, breastfeeding, the menstrual cycle, and menopause can all impact your desire for sex.
YOUR SEX HORMONES
Your body produces three hormones—chemical messengers—that influence your sex drive.
- Estrogen is known as the female sex hormone. It helps to regulate the menstrual cycle and thickens the lining of the uterus every month, and it’s responsible for the growth of female sexual organs. Having higher levels of estrogen can increase sexual desire and vaginal lubrication. This is in part responsible for women’s mid-cycle surge in libido near ovulation.
- Progesterone works in conjunction with estrogen to manage the menstrual cycle and either slough off the thickening uterine lining every month if you haven’t conceived or support a pregnancy if you have. Having higher levels of progesterone tends to reduce sexual drive.
- Testosterone is known as the male sex hormone, but it’s also produced in small quantities by women. Its main function is believed to be in fueling sexual desire.
WHEN SEX HORMONE PRODUCTION IS LOW
Many postmenopausal women experience a dip in sexual desire related to their lesser production of estrogen and testosterone, which occurs naturally with aging. In younger women, stress can inhibit testosterone production, while breastfeeding stalls estrogen production. All three conditions can impact a woman’s sexual response.
ESTROGEN HORMONE THERAPY
Although estrogen replacement had been linked to an increased risk of cardiovascular disease and cancers, a landmark new study demonstrates no rise in risk for women using topical estrogen for relief of genitourinary syndrome.
- The nearly 20-year follow-up study of 53,000 nurses, which was published in December, 2018, found that despite its “black box” warning, low-dose vaginal estrogen does not increase risk.
- “It’s really important to differentiate between systemic estrogen replacement and topical estrogens,” says UCI Health urogynecologist Felicia Lane. “This new study shows that topical applications — unlike systemic estrogen replacement — do not increase the risk of blood clots, cardiovascular disease, osteoporosis or breast and endometrial cancers.”
- If you still have a uterus, you should take progesterone with estrogen to prevent the overgrowth of your uterine lining, which can lead to uterine cancer.
- The US Food and Drug Administration (FDA) says there’s no evidence that hormone therapy increases sex drive.
- Women who are not candidates for vaginal estrogens—those who’ve had breast cancer or a recent stroke—may consider non-estrogen lubricants such as Vitamin E suppositories. If this is your category, have a conversation with your doctor about what is right for you.
TESTOSTERONE HORMONE THERAPY
Taking small doses of testosterone to fuel desire is controversial in women, since it can cause hair growth, acne, and deepen the voice. The long-term safety of using testosterone products—creams, gels, patches, or pills—is also unknown. And there is no testosterone product that is specifically approved by the FDA for use in women to improve the sex drive, so doctors must prescribe a product made for men “off-label.”
A NON-HORMONAL OPTION
A convenient and innovative option after childbirth or menopause is the vFit device. The first of its kind, you use vFit in the privacy of your own home every other day for a few minutes to improve sexual function. This device can help increase natural lubrication and improve sensation, pelvic floor strength and control—all while at home.
Article Provided By Our Partners at Joylux

 PODCAST LISTEN LIVE
PODCAST LISTEN LIVE


